Clinically Isolated Syndrome (CIS)

Models used for illustrative purposes only.
Indications
BETASERON® (interferon beta-1b) is a prescription medicine used to treat relapsing forms of multiple sclerosis (MS), to include clinically isolated syndrome, relapsing-remitting disease, and active secondary progressive disease, in adults.
What is CIS?
Clinically isolated syndrome (CIS) is a first episode of neurologic symptoms caused by inflammation in the central nervous system (CNS). The episode must last for at least 24 hours and is considered a relapsing form of multiple sclerosis (MS). In fact, CIS is often referred to as early MS.
Inflammation in the CNS happens when your body’s immune system mistakenly attacks and damages the protective coating around your nerves, which is called myelin. This damage prevents your nerves from sending signals to your brain, spinal cord, and other parts of your body the way they should.
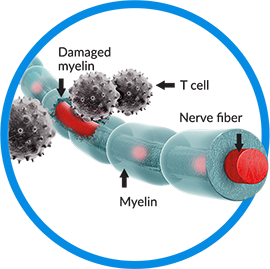
What happens during a CIS episode?
The location where the damage to the myelin occurs in the CNS will determine what symptoms you might experience during a CIS episode. Damage can be in the spinal cord, optic nerve, or brain.
In the spinal cord, the onset of symptoms may be sudden, developing over 1 to 2 hours, or more gradual, happening over a week or more. Symptoms can include muscle weakness; abnormal sensations in the toes and feet; numbness or tingling in the arms, legs, or face; bladder and bowel problems; or Lhermitte’s sign (an electric shock-like sensation when the neck is moved that is felt down the spine, and often into the arms and legs).
In the optic nerve, the onset of symptoms may be sudden or develop over a few hours. Symptoms can include blurred vision or loss of sight, pain behind the eyeball, impaired color or blind spots surrounded by an area of normal vision or other eye problems.
When damage to the myelin occurs in the brain, symptoms may include nausea, vomiting, double vision, dizziness, hearing loss, or problems with balance or walking.
How is CIS diagnosed?
To make a diagnosis of CIS, your doctor—most likely a neurologist—may perform:
Occasionally, your doctor may perform a spinal tap to look at the fluid that surrounds your brain and spinal cord.
How is CIS treated?
In some cases, treatment with a high-dose oral or intravenous (IV) steroid is recommended to reduce symptoms caused by inflammation. Disease-modifying therapy (DMT) is recommended when CIS is considered more likely to progress. The goal of using DMT is to delay a second episode.
Early treatment may lessen the chance of the disease progressing because of additional damage to nerve cells. Beginning treatment with DMT as soon as possible is recommended for patients who have CIS and have MRI results consistent with more advanced types of relapsing MS.
What is the difference between CIS and RRMS?
Patients who experience CIS may or may not progress to other forms of relapsing MS. Relapsing-remitting multiple sclerosis (RRMS) is the most common form of relapsing MS (85% of patients).
In both CIS and RRMS, damage to the myelin interferes with the way the nerves and signals, which causes similar neurology symptoms. The main difference, however, is that a person with CIS has only experienced a first episode, while someone with RRMS has had more than one.
With CIS, MRI results may show damage in the area of the brain that is responsible for the current symptoms. In RRMS, the MRI scan may show multiple lesions (areas of damage) in different areas of the brain. When the MRI scan shows that another episode occurred in the past, the person may be diagnosed with RRMS.
Does CIS always progress?
Not all people who experience CIS will go on to develop RRMS. An MRI scan is one of the most important tools used to identify the risk of disease progressing. Studies have shown there is a high risk of developing RRMS when CIS is accompanied by brain lesions that are similar to those seen in other relapsing forms of MS. When this is the case, patients have a 60% to 80% chance of a second episode and diagnosis of RRMS within several years.



